Care supported by medical science
Physical and emotional pain changes not only the patient's life, but also the life of their loved ones.

Clinical perspective
At Fibroclinic, we know every family wants to see their loved one active, present, with energy, and with the desire to live fully again.
Transcranial Magnetic Stimulation (TMS) is now a real, evidence-based therapeutic option within a human, comprehensive care model.

- Evidence-based protocols with medical oversight
- Integrated interdisciplinary treatment planning
- Continuous follow-up to adjust care safely
Explore TMS by topic
Use these sections to review key clinical information in a clearer, step-by-step format.
What is TMS technology?
Transcranial Magnetic Stimulation (TMS) is an advanced medical technology that uses focused magnetic fields to stimulate specific brain regions involved in pain control, mood, and neuromuscular function.
TMS is a procedure that is:
- Non-invasive
- Painless
- Safe
- Performed without anesthesia or hospitalization
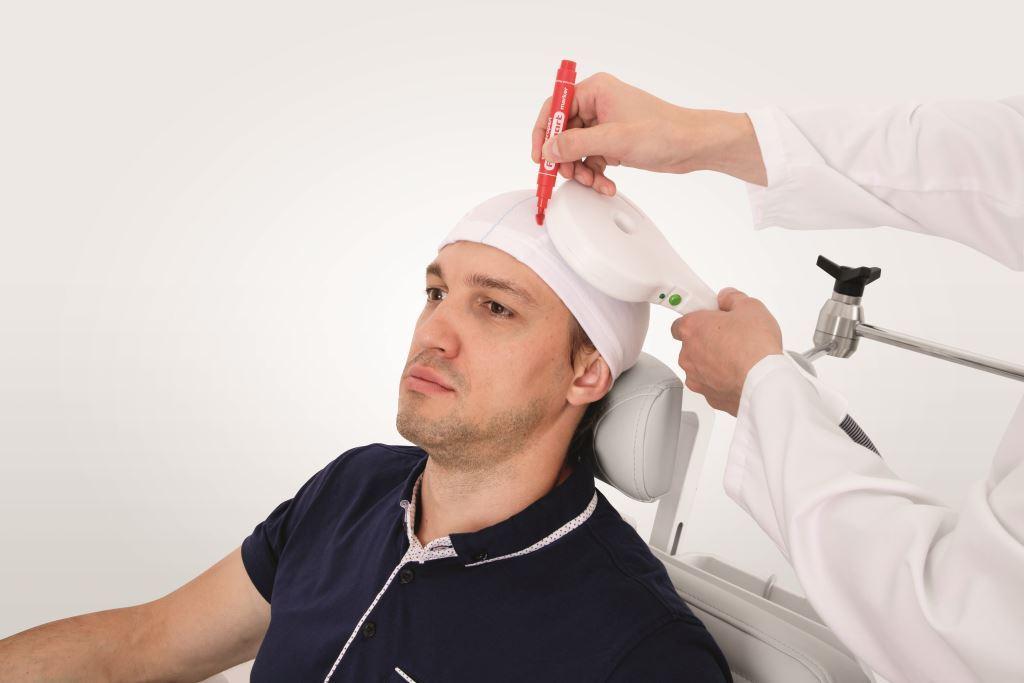
TMS modulates altered brain activity and supports neural regulation processes that can lead to clinical and functional improvement.
International certification and validation
TMS technology has international recognition from institutions such as the FDA, the American Psychiatric Association, and the World Health Organization, and is used in reference medical centers across Europe and North America.
FDA-approved applications (United States):
- Treatment-resistant depression
- Depression with comorbid anxiety
- Obsessive-compulsive disorder (OCD)
- Substance use support, including smoking cessation
- Selected migraine protocols
Additional recognition:
- Recognized by the American Psychiatric Association and WHO as a safe, evidence-based complementary therapy
- Implemented in high-complexity pain, neurorehabilitation, and mental health clinics worldwide
Alternative applications under clinical research
Some conditions currently show promising results in clinical research, but still do not have formal FDA approval for that specific indication.
- Fibromyalgia
- Neuropathic pain
- Migraine (FDA approved in 2013 for specific protocols)
- Autism spectrum disorders
- Tinnitus
- Post-stroke rehabilitation
In these cases, TMS is considered individually under strict medical criteria and always as a complementary therapy, never as a replacement for conventional treatment.
Adverse effects and safety profile
TMS is usually highly tolerated and has an excellent safety profile. Most patients report no adverse effects.
Reported effects may include:
- Mild dizziness, lightheadedness, or temporary fatigue
- Mild local discomfort at the stimulation site
- Neck discomfort from maintaining one position during sessions
Very rare events (<1%), including seizures, have been reported.
TMS as part of an interdisciplinary approach
At Fibroclinic, TMS is not treated as an isolated solution. It is integrated into a complete medical plan coordinated by an interdisciplinary team.
- 1
Rheumatology
Supports reduced pain perception in refractory fibromyalgia, arthritis, and chronic musculoskeletal pain syndromes.
- 2
Psychiatry
Supports improvement in refractory major depression, anxiety, panic symptoms, and post-traumatic stress through targeted circuit modulation.
- 3
Neurosurgery and Neurology
Participates in neuropathic pain, refractory migraine, and complex nerve injury management.
- 4
Physiatry and Physical Therapy
Supports functional recovery, mobility, coordination, and the reinforcement of physical rehabilitation outcomes.
Meaningful improvement is achieved when technology is combined with medical judgment, clinical follow-up, and continuous therapeutic support.
Results patients may experience
After completing a TMS cycle, many patients report:
- Lower chronic pain intensity
- Improvement in depressive and anxiety symptoms
- Better sleep quality
- Greater functional capacity and mobility
- Overall wellbeing and quality of life
Every response is different, and ongoing medical follow-up is essential to adjust the treatment plan to each patient.
Why the clinical evaluation appointment matters
Before starting TMS, a specialized medical evaluation is essential because every brain, diagnosis, and clinical history is different.
At Fibroclinic, this evaluation is performed by Dr. Kathy Fowler, psychiatrist with international Harvard Medical certification in Transcranial Magnetic Stimulation (TMS). During consultation, Dr. Fowler:
- Performs a comprehensive clinical analysis
- Evaluates current diagnosis and previous treatments
- Listens to patient and family goals
- Defines realistic TMS treatment scope for each case
- Determines whether TMS is a safe and appropriate option
Based on this assessment, she prescribes a personalized TMS protocol aligned with each patient's clinical needs and Fibroclinic's interdisciplinary model.
This appointment is key to setting clear, safe, and realistic expectations and integrating TMS into a complete therapeutic plan.
Preparation and expectations
For an appropriate assessment, patients are encouraged to bring their medication list, recent studies, and recent discharge summaries.
TMS is not a single or immediate cure. It is a powerful therapeutic tool that can make a real difference when integrated into interdisciplinary care. At Fibroclinic, the goal is not only to treat symptoms, but to support recovery processes with science, medical judgment, and humanity.
- Response to TMS varies between patients based on diagnosis, clinical condition, disease duration, and adherence to the comprehensive treatment plan.
- TMS does not guarantee 100% effectiveness and does not replace medical evaluation, pharmacologic treatment, or therapies indicated by the treating team.
Ready to start your TMS evaluation?
Book your specialized consultation and receive an evidence-based, personalized interdisciplinary treatment plan.